AMH Levels by Age: Normal Range Chart for Indian Women

If you've recently had an AMH test or your doctor has suggested one, you probably have questions. It's one of the first things we look at when assessing fertility, and for good reason. AMH is a simple blood test that gives us a sense of your ovarian reserve, and while the result might just look like a number on a report, it actually carries quite a bit of information.
What is even more important than the result of the test itself is its interpretation. Your age, medical background, and position on the way to conception will have an impact on this matter.
What Is AMH and Why Does It Matter for Fertility
AMH (Anti-Mullerian Hormone) is the name of a hormone that is secreted from your ovaries through your small follicles. The amount of AMH remains relatively constant during the menstrual cycle, so the test can be taken at any point during the cycle.
Higher AMH levels generally suggest a better ovarian response during IVF treatment, while lower levels may indicate a reduced response. However, AMH does not reflect egg quality, which is also an important factor for pregnancy.
AMH Levels by Age: Normal Range Chart for Indian Women
AMH naturally declines with age. The table below reflects general reference ranges used in clinical practice, including data from large-scale studies conducted across Indian fertility centres.
| Age Group | AMH Level (ng/mL) | What It Indicates |
|---|---|---|
| 20 to 25 years | 3.0 to 4.5 | Strong ovarian reserve |
| 26 to 30 years | 2.5 to 4.0 | Good reserve, optimal fertility window |
| 31 to 35 years | 1.5 to 3.0 | Adequate, mild decline beginning |
| 36 to 40 years | 1.0 to 2.0 | Moderate decline, timely assessment advised |
| 41 to 45 years | Below 1.0 | Low reserve, specialist guidance recommended |
These values are reference ranges, not cut-offs. Individual variation is significant, and a number outside this range does not automatically determine whether conception is or is not possible.
What Is a Good AMH Level to Get Pregnant
The general "good" range for natural conception is considered to be 1.0 to 4.0 ng/mL. For IVF, a level above 1.6 ng/mL is associated with a better ovarian response to stimulation, though pregnancies do occur at lower values with the right protocol.
Age matters as much as the number itself. A 38-year-old with an AMH of 1.8 ng/mL and a 28-year-old with the same reading are in very different clinical positions. Egg quality, which declines with age independently of AMH, plays an equally decisive role in outcomes.
If you’re just exploring your options, you might also think about egg freezing or fertility preservation, especially if your levels are okay right now but you’re worried about how they might change later.
How AMH Levels Affect Your IVF Success at Nova IVF
At Nova IVF, AMH is a clinical tool, not a filter. Specialists use it alongside antral follicle count and age to personalise stimulation protocols across 120+ centres in 75 cities.
With protocols aligned to IVI, one of the world's largest fertility networks, low AMH patients receive adjusted dosages and optimised lab handling rather than a default to donor cycles.
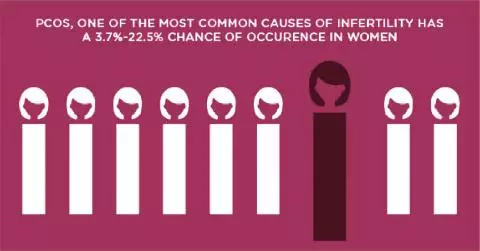
High AMH, often linked to PCOS, is managed through Nova's dedicated PCOS Clinic to prevent hyperstimulation. Every cycle is built around the individual, not a standard template.
How to Increase AMH Levels Naturally: Diet, Lifestyle and Supplements
AMH levels cannot be elevated to a high degree, some actions can help keep the ovarian system operating properly and extend its youthfulness:
- Diet: Foods with antioxidants like fruits, vegetables, and nuts have a protective effect on the eggs against oxidants.
- Vitamin D: Individuals with low vitamin D levels may have experienced a reduction in their AMH levels. Getting enough sunshine and consuming vitamin D-rich foods can help balance the necessary hormones.
- Avoid smoking and alcohol consumption: Both of these activities can make ovaries age faster.
- Exercise: It helps regulate hormones while not stressing the body.
- Supplements: CoQ10 and DHEA supplements are often prescribed in reproductive medicine for enhancing fertility.
FAQs
1. What is a good AMH level to get pregnant naturally?
Generally, 1.0 to 4.0 ng/mL is considered adequate. But age and egg quality matter just as much as the number.
2. Can I still do IVF if my AMH is very low?
Yes, absolutely. Low AMH affects how many eggs are retrieved, but many women still conceive with the right protocol.
3. Does AMH level change month to month?
No. AMH is one of the most stable hormones and stays consistent across your cycle and between months.
4. Is a low AMH level normal after 35 for Indian women?
Some decline after 35 is expected. Indian women may experience it slightly earlier, so testing after 30 is worth considering.
 Infertility Counselling
Infertility Counselling Female Infertility Treatment
Female Infertility Treatment Andrology Treatment
Andrology Treatment Fertility Enhancing Surgeries - Female
Fertility Enhancing Surgeries - Female Fertility Enhancing Surgeries - Male
Fertility Enhancing Surgeries - Male Endoscopy Treatment
Endoscopy Treatment IUI Treatment
IUI Treatment IVF Treatment
IVF Treatment ICSI Treatment
ICSI Treatment Advanced IVF Solutions
Advanced IVF Solutions Embryology
Embryology Vitrification Egg, Embryo, Sperm Freezing
Vitrification Egg, Embryo, Sperm Freezing Preimplantation Genetic Testing (PGT)
Preimplantation Genetic Testing (PGT) Donation Program Embryo / Egg / Sperm
Donation Program Embryo / Egg / Sperm Self-cycleTM IVF
Self-cycleTM IVF

 Self-cycleTM IVF
Self-cycleTM IVF