Success story of Azoospermia And Severe OAT (Male Infertility) conceived through IVF- ICSI
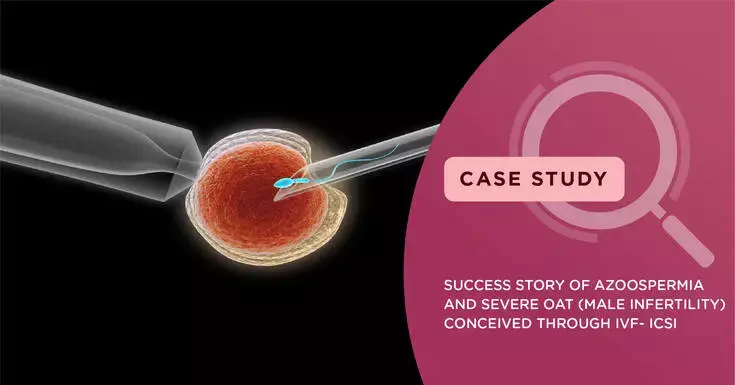
Successfully helping a couple with Azoospermia and Severe OAT conceive their own biological child
A couple visited Nova IVF Fertility, Chennai to consult about their fertility issue with Dr. Madhupriya. Both husband and wife were initially advised to undergo the routine fertility tests. The wife’s cycle and hormonal analysis were normal, but the husband’s semen analysis revealed a case of Azoospermia and severe OAT. The male had very few motile sperms.
Understanding Azoospermia and Severe Oligoasthenoteratozoospermia (OAT)
Men who don’t have any sperm in their semen suffers from a condition called Azoospermia. It impacts about 1% of men and it can be the reason for infertility for about 15% of infertile men.
Such men will not be able to use their own semen to make their partner pregnant unless they are treated for the specific cause and get it rectified. If nothing works out, another potential treatment choice is to use a sperm donor.
One of the possible reasons for Azoospermia is the testicles being unable to make sperm or a condition that prevents sperm from getting out of the body.
There are three main types of Azoospermia:
- Pretesticular Azoospermia: Testicles are normal, but not producing any sperm. It is a very rare condition that might happen because of low hormone levels or after chemotherapy.
- Testicular Azoospermia: Damage to testicles stops them from making sperm normally. It can happen because of an infection in the reproductive tract, such as epididymitis and urethritis or a childhood illness such as viral orchitis, causing swelling of one or both testicles. Additional causes include a groin injury, Cancer or its treatments, like radiation and genetic conditions, such as Klinefelter’s syndrome.
- Post-testicular Azoospermia: Testicles make normal sperm, but something prevents from getting out, e.g. vasectomy, a blockage, (called obstructive Azoospermia) impacting the tubes that carry sperm from testicles to penis or retrograde ejaculation, in which the semen goes back into the bladder instead of out of the penis. About 40% of men with Azoospermia have the post-testicular type.
Diagnosis involves testing of sperms, and if there is a complete absence of sperms, the medical history is checked, and physical, and blood tests are conducted to check the hormone levels. If hormone levels are normal, a scrotal or transrectal ultrasound is performed to look for obstruction(s) in the vas deference. An MRI may confirm the diagnosis. Sometimes, surgery is the only way to locate the obstruction. If there is no blockage, genetic tests are required to identify genetic conditions.
Treatment options for Azoospermia include treatment with certain hormones, coaxing sperm back to semen or increasing the likelihood of finding sperm during extraction. These hormones include Follicle-stimulating hormone (FSH) and Human chorionic gonadotropin (HCG).
Sperm retrieval is performed for men with non-obstructive Azoospermia or those who have a blockage but don’t want surgery. A tiny needle is used to draw sperms directly from the testicle and the sample subsequently frozen for use later for IVF treatment.
Oligoasthenoteratozoospermia (OAT) is a condition that includes oligozoospermia (low number of sperm), asthenozoospermia (poor sperm movement), and teratozoospermia (abnormal sperm shape). OAT is the commonest cause of male subfertility.
Treatment Suggested by Dr. Madhupriya, Fertility Specialist
The patient was advised an option of pulling motile sperm from the ejaculate or a testicular aspiration if needed. They were counselled to go ahead with ICSI after subjecting the sperm to HOS and selecting the motile sperm.
Hypo Osmotic Swelling (HOS) Test
The hypo osmotic swelling (HOS) test is a relatively new assay used to evaluate the functional integrity of the sperm’s plasma membrane and useful addition to routine semen analysis. This is a good sperm indicator that can help manage fertility outcomes better.
Factors monitored in the HOS test include progressive motility, morphologically normal spermatozoa, percentage of swelling with the hypo‐osmotic test. The hypo‐osmotic test provides a simple evaluation of membrane function and the results obtained show that those with low swelling scores (<40%) to be of doubtful fertility.
Intracytoplasmic Sperm Injection (ICSI)
Intracytoplasmic sperm injection is an IVF procedure in which a single sperm cell is directly injected into the cytoplasm of an egg. This technique is used for preparing the gametes to obtain embryos which can be transplanted into the maternal uterus. The most important indicator of ICSI success is the fertilisation rate achieved. Typical fertilisation rates are exceptional and in the ranges of 80 to 85 per cent. In this process, one selected sperm is injected into the cytoplasm of an individual oocyte (egg).
Apart from an exceptionally high fertilisation rate, an added advantage of this procedure is that a clean and washed sperm sample can be prepared using multiple techniques in order to eliminate poor quality sperm, thereby using a very high-quality sperm for IVF.
Successful Treatment Outcome
IVF cycle was initiated for the lady. Sperm sample was retrieved through the aspiration technique and was subjected to the washing procedure. The HOS positive sperms were used for carrying out the ICSI procedure and injected into the cytoplasm of the twenty eggs that were retrieved from the female partner.
9 of these eggs were fertilised, and 2 blastocysts were formed. Both the blastocysts were transplanted into the uterus of the lady.
The couple sub sequentially conceived with twins. Everything went well, as expected, during the pregnancy period, and the couple was blessed with their own biological twins.
 Infertility Counselling
Infertility Counselling Female Infertility Treatment
Female Infertility Treatment Andrology Treatment
Andrology Treatment Fertility Enhancing Surgeries - Female
Fertility Enhancing Surgeries - Female Fertility Enhancing Surgeries - Male
Fertility Enhancing Surgeries - Male Endoscopy Treatment
Endoscopy Treatment IUI Treatment
IUI Treatment IVF Treatment
IVF Treatment ICSI Treatment
ICSI Treatment Advanced IVF Solutions
Advanced IVF Solutions Embryology
Embryology Vitrification Egg, Embryo, Sperm Freezing
Vitrification Egg, Embryo, Sperm Freezing Preimplantation Genetic Testing (PGT)
Preimplantation Genetic Testing (PGT) Donation Program Embryo / Egg / Sperm
Donation Program Embryo / Egg / Sperm















Add new comment