Blastocyst Culture in IVF: Understand its Stages and Benefits
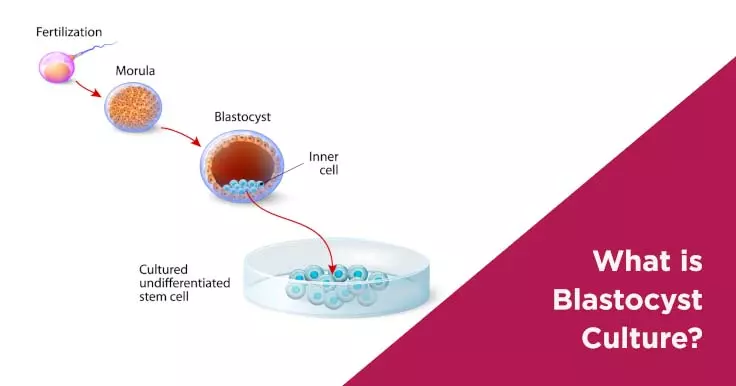
In the IVF laboratory, after the egg retrieval procedure, fertilization is carried out by IVF (In-vitro fertilization) or by ICSI (intra-cytoplasmic sperm injection) and the resulting embryos are placed in an incubator for further development. The stages of development are as follows:
- The day of egg retrieval is considered as Day 0 (IVF or ICSI is done after egg retrieval)
- The pronuclear stage on day 1 (embryologist checks as to how many eggs have successfully fertilised)
- The two to four cell stage on Day 2
- The eight cell stage on day 3
- The morula stage on day 4
- The blastocyst stage on day 5 or day 6
The blastocyst contains two different cell types- the inner cell mass which develops into the fetus, and an outer layer of cells called trophectoderm which develops into the placenta.
Historically, embryo transfer following IVF or ICSI has been carried out on Day 2 or Day 3 after egg collection. However, advances in the IVF laboratory advances allow us to now culture embryos for five or six days. This gives the embryos more opportunity to prove their developmental potential. Some embryos stop developing (arrest) prior to day 5/6. This 'natural selection' enables the embryologist to identify and choose the best embryo/s for embryo transfer.
Advantages of Blastocyst Culture
Blastocyst culture requires optimal laboratory conditions. On an average, about 45% of fertilized eggs reach the blastocyst stage.
As only the embryos with the best development capacity become blastocysts, allowing embryos to grow and develop in the laboratory till they reach the blastocyst stage allows the selection of the most competent embryo/s for embryo transfer.
Also, in a natural pregnancy, it takes around five days after fertilisation for the embryo to reach the womb, where it then implants. The lining of the uterus is particularly receptive on this day. Performing blastocyst transfer hence is more physiological.
Some couples require PGS (pre-implantation genetic screening) or PGD (pre-implantation genetic diagnosis). For them, blastocyst culture is required as embryo biopsy is recommended to be done in blastocyst stage rather than on Day2/3 embyos.
Who Can Benefit from Blastocyst Culture?
Blastocyst culture is advised for:
- For patients with multiple failed IVF: Performing a blastocyst culture on a patient with a history of failed IVF with day2/3 embryo transfer, can yield more information related to the growth of the embryos and aid in improving pregnancy rate
- To eliminate multiple pregnancies: Blastocyst culture allows the possibility of transferring the single best embryo and thereby reducing the chance of multiple pregnancy.
Are there any drawbacks to blastocyst transfer?
Not all clinics perform blastocyst culture. Quality control and optimal laboratory culture conditions are essential for successful blastulation.
There is a risk that none of the embryos become blastocysts. In that case the embryo transfer procedure gets cancelled. In good IVF laboratories, this usually means that probably none of embryos were competent enough to reach blastocyst stage and performing a day3 transfer also probably would not have led to a pregnancy.
Since fewer embryos become blastocyst, there maybe fewer or no surplus embryos to freeze after the initial embryo transfer in the fresh cycle. But, since success rates are better with a blastocyst transfer than with day3 transfer, a frozen may not be needed after all.
Should all patients go ahead with a blastocyst transfer?
Depending on factors like age, medical history and number and quality of embryos, it may be better to transfer a day3 embryo, particularly for women in their first IVF cycle.
 Infertility Counselling
Infertility Counselling Female Infertility Treatment
Female Infertility Treatment Andrology Treatment
Andrology Treatment Fertility Enhancing Surgeries - Female
Fertility Enhancing Surgeries - Female Fertility Enhancing Surgeries - Male
Fertility Enhancing Surgeries - Male Endoscopy Treatment
Endoscopy Treatment IUI Treatment
IUI Treatment IVF Treatment
IVF Treatment ICSI Treatment
ICSI Treatment Advanced IVF Solutions
Advanced IVF Solutions Embryology
Embryology Vitrification Egg, Embryo, Sperm Freezing
Vitrification Egg, Embryo, Sperm Freezing Preimplantation Genetic Testing (PGT)
Preimplantation Genetic Testing (PGT) Donation Program Embryo / Egg / Sperm
Donation Program Embryo / Egg / Sperm Self-cycleTM IVF
Self-cycleTM IVF

 Self-cycleTM IVF
Self-cycleTM IVF